History
A 55 year old female attended the clinic for consultation regarding treatment of metastatic ovarian carcinoma.
She was diagnosed 2 1/2 years previously after biopsy of an enlarging lymph node in the neck was found to be metastatic ovarian carcinoma. The patient was treated initially with hysterectomy and bilateral salpingo-oophorectomy with omentectomy, followed by chemotherapy with paclitaxel (Taxol) and carboplatin. Six cycles were successfully completed, and resulted in a complete remission.
The patient was feeling well for about 1 year, when there was disease recurrence (another new neck node was found). She was then treated with liposomal doxorubicin (Caelyx) plus carboplatin. Due to incomplete response, this was followed by re-treatment with paclitaxel (Taxol) alone for 8 cycles. While receiving paclitaxel, the CA-125 began rising so it was stopped. She came to see us 2 months following the last dose of chemotherapy.
The patient had a history of pneumonia and kidney infection but was otherwise healthy. She has a 30 year smoking history. She was taking some vitamins, an OTC anti-histamine (as needed) and a beta-glycan supplement. She had some environmental allergies, and a sulfa allergy. Aside from bilateral leg edema, she was feeling well.
Findings
On examination, vital signs were normal: BP = 120/77, HR = 76, SpO2 = 96 on room air. Body weight was 66kg. A small left supracalvicular mass was palpable. There was mild bilateral ankle edema, and no calf tenderness or erythema. Abdomen revealed a laparotomy scar, no masses or liver enlargement. The remainder of the examination was normal.
Treatment
We recommended a combination of DCA + TM. The DCA dose was 500mg p.o. t.i.d. (23mg/kg/day) on cycle of 2 weeks on / 1 week off. We supplemented this with R-alpha lipoic acid 150mg t.i.d. and benfotiamine (vitamin B1) 80mg twice a day. TM was started at 20mg 6 times a day. Appropriate weekly blood tests were ordered. CA-125 at treatment start was 38.3 (normal less than 35).
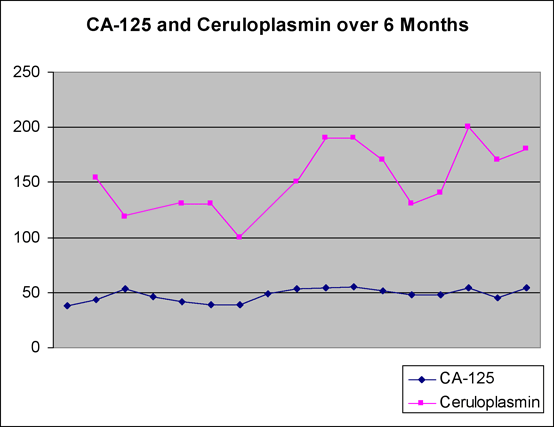
The patient tolerated both DCA and TM very well. There only significant side effect was a drop in red and white cell counts when copper was depleted from the body with TM. This patient was quite sensitivity to copper deficiency, and the drop in cell counts resulted in difficulty maintaining a consistent low ceruloplasmin level. See graph below. TM dose was adjusted on a weekly basis to reduce ceruloplasmin without causing an excessive drop in blood cell counts. The average TM dose was 20mg t.i.d.
Despite this, the cancer came under control with DCA+TM treatment. The CA-125 increased slightly at the start of treatment as expected because of the 4-8 weeks it takes to create maximum copper deficiency. The CA-125 fluctuated slightly, but remained in the range of 39-55 for the next 6 months (Fig. 8A).
Fig. 8A – CA-125 values with DCA + LDN treatment
CT scanning done 2 months into treatment revealed stable disease (Fig. 8B).
Fig. 8B – comparison with CT 2 months prior showing stable disease (some lymph nodes smaller by 2-3 millimeters and some larger by 1-2 millimeters, no new metastases)
After 4 months of treatment CT scans were again repeated. The result was once again stable disease (Fig. 8C).
Fig. 8C – CT scan showing stable disease after 4 months of treatment
After 5 months of treatment, the patient began to develop mild numbness in the toes of both feet. Since we were concerned about the possibility of neuropathy from DCA, we decided to stop the DCA and arrange nerve conduction testing. The patient elected to try noscapine with TM while off DCA. Within a few weeks of stopping DCA, the CA-125 began to climb reaching a maximum of 112 (approximately doubled after stopping DCA). By this time the numbness had completely resolved and the nerve conduction test was done showing no neuropathy.
DCA was then re-started and the CA-125 began to fall again. The patient became anxious from the rise in CA-125 and decided to switch from DCA+TM to chemo to get the cancer back under control faster. We planned to review the treatment again after 1 or 2 cycles of chemo, and consider going back to DCA+TM at that time.
Comments
This patient was successfully treated with a combination of DCA+TM and experienced stable disease (proven by CA-125 and CT scans) for the entire duration of the treatment which was about 6 months. The main advantage of this treatment was the lack of serious side effects, especially compared to the traditional treatment of chemotherapy.
Changing from DCA+TM to noscapine+TM was not effective, proving the benefit of DCA. The fluctuation of CA-125 along with the ceruloplasmin level also showed that TM was contributing to cancer stabilization.
There was no resistance to DCA or TM. The only reason the treatment was changed was concern about neuropathy which ultimately proved to be false. DCA and TM may be used again in the future with this patient.
For TM treatment, we no longer use TM on a 6 times per day schedule. We find that a double dose given 3 times a day is equally effective at the start of treatment.