History
A 59 year old female presented to us for treatment of metastatic ovarian carcinoma. The patient was diagnosed 4 years previously when she felt an axillary mass, and proceeded to have a biopsy. The initial biopsy showed metastatic carcinoma, but the origin was unclear at the time. Further workup revealed an elevated CA-125 tumour marker. A presumptive diagnosis of ovarian carcinoma was made, and she was offered “palliative” chemotherapy. Since the patient felt generally well, and was very concerned about loss of quality of life with chemo, she refused it. The patient continued to do well for about 2 years with no cancer treatments.
With progression of the cancer, the patient agreed to have surgery (hysterectomy, and salpingo-oophrectomy). Surgical pathology revealed grade 2 bilateral serous ovarian carcinoma with invasion into the fallopian tubes and metastases to the uterus, peritoneum and omentum. The patient recovered quickly from the surgery. She was again offered chemotherapy, but declined. A few months later, she developed difficulty breathing and a right pleural effusion was diagnosed. Right thoracentesis and pleurodesis were carried out. CA-125 was stable for about 3 months after that, but then a rise prompted her to seek additional treatment. Two months prior to seeing us, the patient had a CA-125 of 183.
The patient was previously healthy and a non-smoker. She complained of low energy, nausea, diarrhea, exertional dyspnea and intermittent palpitations. She had already been investigated by a cardiologist for the breathing problem and palpitations but nothing unusual was found. She also had a new pain with a burning quality in the left inguinal region. She was taking Imodium as needed for the diarrhea, and Gravol for nausea. She had Tylenol #3 at home but reported it was not effective for the inguinal pain.
Findings
The patient’s body weight was 41kg. There was no cachexia. Vital signs were normal. Oxygen saturation was 98% at rest and with exertion. A few mobile and non-tender lymph nodes (about 0.5cm) were palpable in the cervical chains bilaterally. There was a hard left inguinal node (about 1.0cm). There was no abdominal distension. The rest of the examination was normal.
Treatment
The patient stated that she did not want any chemotherapy except as a last resort. She only wanted to try gentler therapies first. She chose to try DCA + LDN as her initial treatment. She was started on DCA 500mg daily as a test dose. The dose was raised to 500mg b.i.d.(25mg/kg/day) since she tolerated it well. Her treatment cycle was 2 weeks of DCA followed by a 1 week off. She was instructed to take benfotiamine 80mg b.i.d. and R+SR Alpha Lipoic Acid 150mg t.i.d. She was given pantoprazole 40mg q.d. as needed to prevent GI upset from DCA. The initial LDN dose was 3mg qHS which was to increase to 4mg qHS after 2 weeks if tolerated. Lyrica was also started for pain management.
There was a clear symptomatic response to treatment. Within 2 weeks, the nausea had improved and the diarrhea which had been present for months had resolved. Pains were markedly improved. CA-125 dropped from 183 to 155. By 4 weeks, the patient had gained about 5 lbs and was back to her pre-cancer weight. There was no edema or ascites. After 4 weeks of treatment, her CA-125 began to rise gradually (see figure 5A).
Since the response to treatment was diminishing, a change in treatment was recommended. The patient wished to continue with DCA to see if the rise in CA-125 was just temporary. At 8 weeks of treatment, the DCA was increased to 500mg t.i.d. (37mg/kg/day). At 12 weeks, she began to develop nausea again and also developed numbness in the toes bilaterally along with mild hallucinations. At that point it was clear the DCA was causing side effects and was no longer beneficial. A CT scan was performed at this time confirming mild tumour growth. See Fig. 5A and 5B.
Fig. 5A – CA-125 values with DCA + LDN treatment
| 2 months pre-treatment | Start | 2 wks | 4 wks | 6wks | 8 wks | 12 wks | |
| CA-125 | 183 | unknown | 166 | 155 | 204 | 263 | 389 |
Fig. 5B – CT Scan Abdomen/Pelvis
At this point the patient chose to switch to anti-angiogenic monotherapy with ammonium tetrathiomolybdate (TM). The starting dose of TM was 20mg 6 times a day. No zinc supplementation was used. The patient’s ceruloplasmin came down rapidly, and she began to develop crampy pains in her leg muscles. Oral magnesium tablets were started and the cramps resolved.
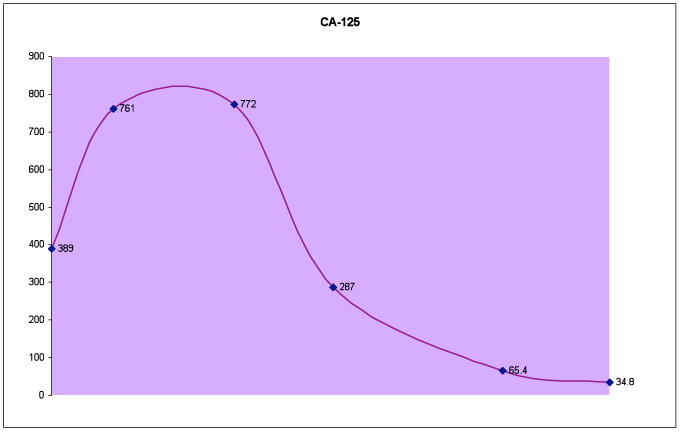
We were able to maintain a ceruloplasmin in the range of 110 – 120g/L with no serious drop of the blood cell counts. CA-125 dropped from a high of 772 to 287 after 3 months of controlled copper deficiency. By 6 months, the CA-125 was down to 34.8.
Fig. 5C – CA-125 level over a period of 6 months
Medications being taken were: TM 20mg t.i.d., Gravol 50mg prn, Magnesium/calcium tablets and Tylenol #2 on occasion.
The patient was feeling well with no nausea, no diarrhea, and minimal pains. A repeat CT scan was done which was reported as “slight increase” in abdominal metastases and “ascites has resolved”. Taking into account the small variance in that the last 2 scans (done at different hospitals) and the large reduction of CA-125, it was concluded that the cancer was stable or improved.
Comments
This case is an example of a partial response to DCA + LDN. Even though the initial response to these drugs was favourable, the effect was reduced after about 1 month. Various scenarios could explain this. It is possible that the combination therapy was not ideal, and that DCA or LDN may have worked better if used independently.
Another possible explanation is that this patient had more than 1 population of cancer cells which responded differently to various treatments. One population of cells may have been killed by DCA+LDN leaving the remaining resistant cells to continue growing.
It is also possible that the cancer cells developed resistance to DCA after being exposed to the drug. Only further research will give us answers to these questions.
This case also confirms that patients may have an excellent long-term response (life extension and quality of life improvement) with a simple treatment like controlled copper deficiency using TM.